|
The choice among the three surgical approaches described herein can be made depending on the patient’s anatomical characteristics and surgeon’s preference. There is no gold standard surgical approach in terms of laparoscopic splenic flexure mobilization. In such cases, surgeons can easily reach splenic flexure by using a port placed in the left upper quadrant. However, laparoscopic instruments cannot always reach splenic flexure in patients with large bodies. Surgeons usually stand on the right side of the patient and use the right side port as the working port. To avoid splenic injury, surgeons do not make extensive traction of the splenic flexure colon because this could result in splenic laceration or omental bleeding. One of the complications in splenic flexure mobilization is splenic injury. In such cases, it is easy to dissect the pancreas from the transverse mesocolon using an anterior approach. In general, surgeons can easily find the pancreas by continuing medial-to-lateral mesocolon dissection however, in obese patients it can be difficult to find the pancreas using an inferior approach because of thick fat tissue around the pancreas. These three surgical approaches of laparoscopic splenic flexure mobilization are feasible and safe. The only goal for splenic flexure mobilization is gaining enough length of the descending colon to enable tension-free anastomosis. In the lateral approach, the phrenocolic and splenocolic ligament is divided, after which the lesser sac is entered from the lateral part (see details in video). In the anterior approach, the lesser sac is entered from the anterior part by dividing the gastrocolic ligament first, while in the inferio-medial approach the lesser sac is entered from the inferior part by dividing the pancreaticocolic ligament first. 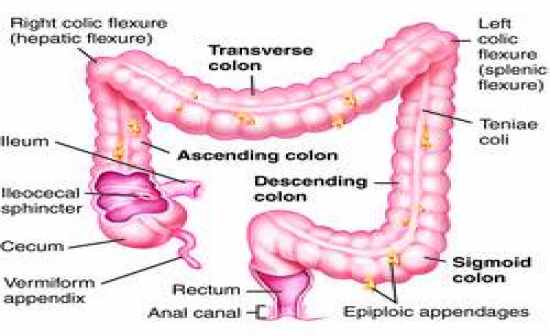
After completion of inferior mesenteric artery (IMA) and inferior mesenteric vein (IMV) ligation and medial to lateral mesocolic dissection, the author started splenic flexure mobilization. 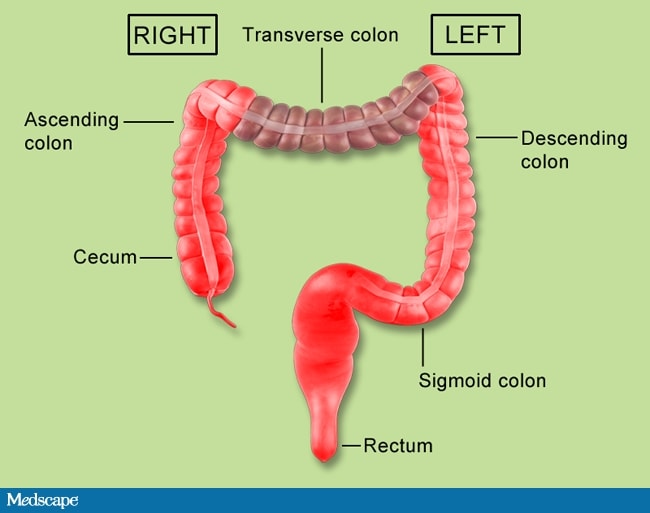
Patients were placed in the supine position with reverse Trendelenburg and right down tilting position. lateral) for laparoscopic splenic flexure mobilization are introduced.Īlthough splenic flexure mobilization occasionally looks complicated, it consists of five simple procedures: 1, division of the line of Toldt (dividing the lateral peritoneal attachment) 2, division of the gastrocolic ligament (dividing the greater omentum and transverse colon, then entering the lesser sac) 3, division of the splenocolic ligament 4, division of the phrenocolic ligament 5, division of the pancreaticocolic ligament (division of the transverse mesocolon and inferior border of the pancreas).īased on the method of entering the lesser sac, laparoscopic splenic flexure mobilization can be categorized into three surgical approaches: A, anterior approach B. Accordingly, colorectal surgeons should be familiar with splenic flexure mobilization however, laparoscopic splenic flexure mobilization can be time-consuming and technically demanding. Splenic flexure mobilization, which is an essential surgical procedure to elongate the left colon, is the only way to induce tension free anastomosis. 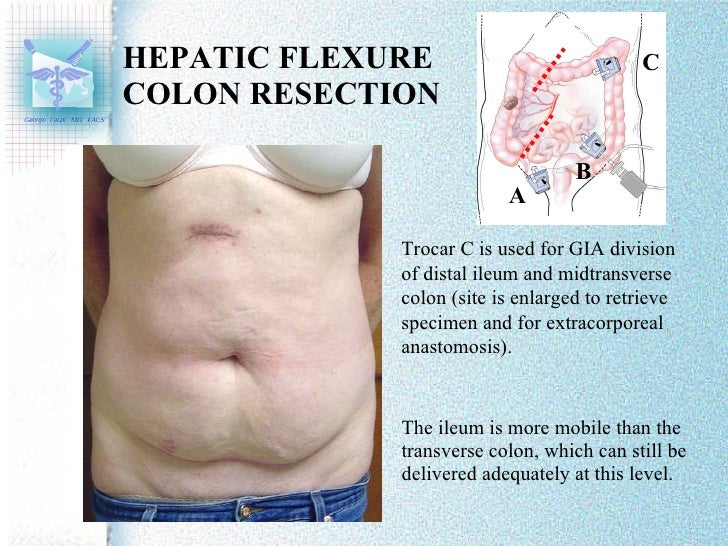
Many factors are associated with anastomotic leakage, among which tension-free anastomosis is one of the most important. 1– 3 One of the most disastrous complications after colorectal surgery is anastomotic leakage. Patients who undergo colorectal laparoscopic surgery generally experience less pain, faster recovery and acceptable oncological outcomes. Laparoscopic surgery has been accepted as an alternative surgical option as well as a better surgical option for treating colorectal cancer based on the results of multicenter prospective randomized trials.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
